To Book an Appointment
Call Us+91 926 888 0303What is Necrosis: Types, Symptoms, and Treatment
By Dr. Namrita Singh in Internal Medicine
Jan 27 , 2026
3
Your Clap has been added.
Thanks for your consideration
Share
Share Link has been copied to the clipboard.
Here is the link https://max-health-care.online/blogs/what-is-necrosis
Necrosis refers to the death of body tissue caused by a lack of blood flow, infection, or injury, leading to the irreversible breakdown of cells in the affected area. This disrupts the function of nearby organs. For example, if it occurs in the heart, it can weaken its ability to pump blood, and if it affects the brain, it can impact important nerve functions. Left untreated, it may spread, cause severe infections, or even lead to sepsis. That’s why it’s so important to spot the early signs and know the different types. This blog takes you through what necrosis really is, what causes it, and how to recognise it before it leads to something more serious. Let’s start with the basics.
What is Necrosis?
Necrosis is the premature death of cells and living tissue in the body, occurring when cells are severely damaged by factors such as injury, infection, lack of blood supply, or exposure to toxins. Unlike the body's normal, controlled process of cell death, necrosis is an unplanned event that happens when cells can no longer survive due to extreme stress or harm. When tissue dies in this way, it can affect any part of the body, from skin and muscles to internal organs, and often requires medical attention because the dead tissue cannot heal on its own and may need to be removed to prevent further complications.
What are the Different Types of Necrosis?
Necrosis can appear in several forms, depending on how and where the tissue damage occurs. Each type has distinct features and underlying causes:
Coagulative Necrosis
Coagulative necrosis is the most common form and usually occurs in organs such as the heart, kidneys, and adrenal glands. It develops when blood flow to a specific area is suddenly cut off, depriving cells of oxygen and nutrients. As a result, the affected tissue becomes firm, pale, and dry, retaining its basic structure for a short time before breaking down. This type is commonly seen after a heart attack or other conditions that block blood supply to an organ.
Liquefactive Necrosis
Liquefactive necrosis often affects the brain and tissues with high enzyme content. It happens when cells are destroyed so rapidly that enzymes released from dying cells break down surrounding tissue into a soft, liquid mass. This type is typical in bacterial infections, abscesses, or strokes affecting the brain, where dead tissue turns into a pus-like fluid.
Caseous Necrosis
Caseous necrosis has a distinct appearance, the dead tissue looks soft and crumbly, similar to cheese. It is most often linked to tuberculosis and certain fungal infections. This form develops when the immune system tries to wall off infectious organisms, creating a mixture of dead cells and inflammatory debris. Over time, this material becomes trapped within a fibrous capsule, forming granulomas that can damage surrounding tissue.
Fat Necrosis
Fat necrosis occurs in fatty tissues such as the breasts, thighs, or pancreas. It often results from trauma or the release of digestive enzymes that break down fat cells. The damaged fat combines with calcium deposits, forming hard, chalky areas within the tissue. In the pancreas, this can occur during pancreatitis, leading to local inflammation and discomfort.
Gangrenous Necrosis
Gangrenous necrosis affects large sections of tissue, particularly in the limbs or intestines. It typically arises when blood supply is severely reduced or completely blocked. The tissue begins to decay, turning black or greenish, and may emit a foul odour. There are two main forms: dry gangrene, caused by poor circulation (often seen in diabetes or vascular disease), and wet gangrene, which involves infection and spreads quickly, posing a serious threat to life if not treated urgently.
Fibrinoid Necrosis
Fibrinoid necrosis mainly involves the walls of blood vessels and occurs in certain autoimmune or severe hypertensive conditions. In this type, immune complexes and proteins like fibrin accumulate within the vessel walls, making them thick, weak, and prone to rupture. Over time, this can lead to bleeding, reduced blood flow, or organ damage depending on which vessels are affected.
What Causes Necrosis?
Necrosis can be triggered by several factors that severely damage or destroy cells and tissues. Common causes include:
- Reduced Blood Supply (Ischaemia): When blood flow to a tissue is blocked or severely reduced, cells are deprived of oxygen and nutrients. This is a common cause of necrosis in the heart, brain, and extremities, often seen in heart attacks, strokes, or peripheral artery disease.
- Infections: Bacterial, viral, or fungal infections can damage tissue directly or trigger inflammation that leads to cell death. Severe infections such as gangrene or abscesses often result in necrosis.
- Physical Injury or Trauma: Accidents, burns, or frostbite can destroy cells in a localized area, leading to tissue death. The severity and extent of necrosis depend on the force and duration of the injury.
- Toxins and Chemicals: Exposure to harmful chemicals, poisons, or certain medications can damage cells and cause necrosis. This includes substances that interrupt normal cellular processes or blood flow.
- Inflammation or Autoimmune Reactions: In some cases, the body’s own immune system attacks healthy tissue, as seen in autoimmune diseases or severe inflammatory conditions. This immune-mediated damage can trigger necrosis in affected areas.
- Obstructions or Pressure: Prolonged pressure on tissues, such as in bedsores, can limit blood flow and oxygen supply, eventually causing necrosis.
What are the Symptoms of Necrosis?
Symptoms can vary depending on the location, type, and severity of the tissue death:
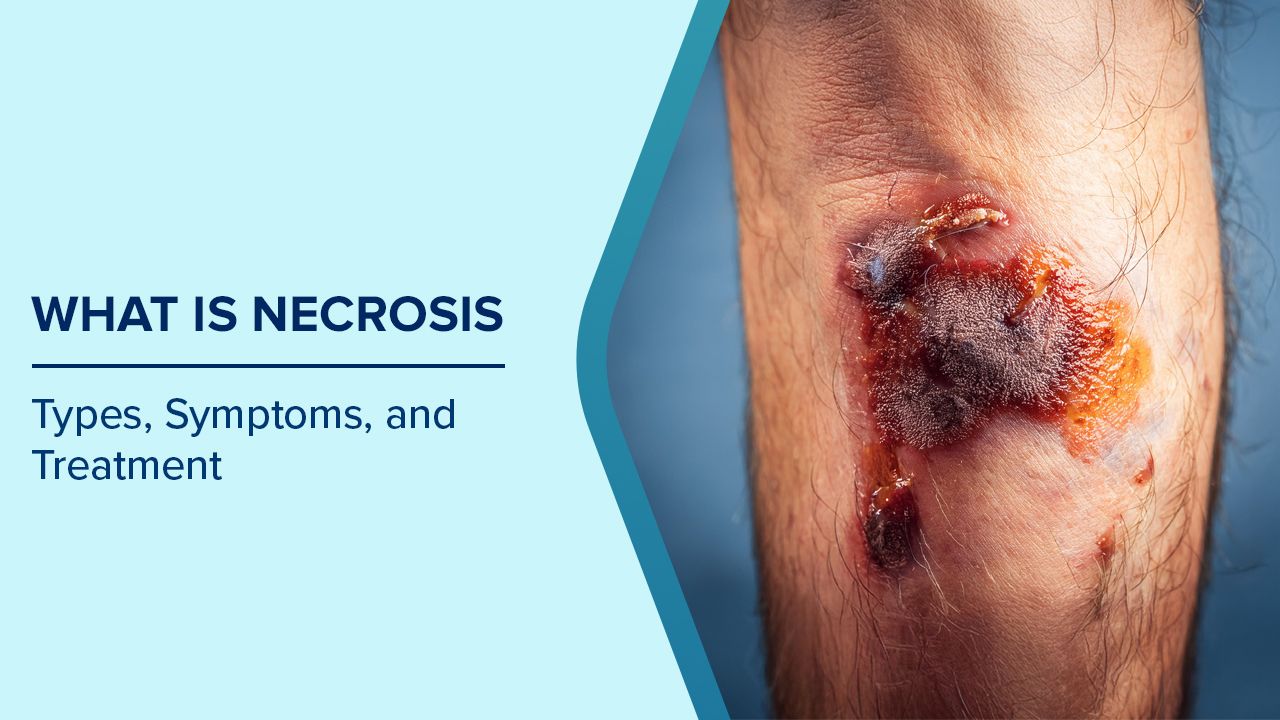
- Changes in Skin and Tissue: The affected area often shows noticeable colour changes, ranging from pale or red to brown or black. Tissue texture can become hard, soft, or even mushy. In some cases, the skin may break down, forming ulcers, blisters, or open wounds. Dead tissue may also emit a foul odour, especially in cases of gangrene. These visual changes are often the first sign that necrosis is occurring.
- Pain and Sensory Changes: Pain is a common symptom and can range from mild discomfort to severe, persistent pain in the affected area. Nerve damage may cause numbness, tingling, or a burning sensation. In certain types of necrosis, the surrounding tissue may feel unusually tender, and any pressure on the area can intensify discomfort.
- Swelling and Redness: Inflammation is the body’s natural response to tissue death. Necrotic areas often swell and appear red or warm to the touch. Swelling can spread beyond the immediate site of necrosis, making the area appear larger and more inflamed.
- Signs of Infection: Necrotic tissue provides a favourable environment for bacteria, increasing the risk of infection. This may lead to pus formation, foul-smelling discharge, or oozing from wounds. Systemic signs such as fever, chills, or general malaise may indicate that the infection is spreading, which can escalate to life-threatening conditions like sepsis if not treated promptly.
- Organ-Specific Symptoms: Necrosis in vital organs can affect their function. For example, heart necrosis may cause fatigue or shortness of breath, brain necrosis can result in weakness, speech difficulties, or memory problems, and necrosis in the liver or kidneys may affect metabolism or fluid balance.
- Systemic Effects: Large-scale or severe necrosis can trigger widespread symptoms such as extreme fatigue, rapid heartbeat, low blood pressure, and signs of systemic inflammation, reflecting the body’s response to dying tissue.
How is Necrosis Diagnosed?
Diagnosing necrosis requires a combination of physical evaluation, imaging studies, and laboratory tests to determine the extent of tissue damage and its underlying cause.
Physical Examination
A doctor usually begins with a thorough examination of the affected area. They assess visible signs such as discolouration, swelling, changes in tissue texture, open wounds, or foul odour. The size, location, and progression of the affected tissue help indicate the type of necrosis and its severity.
Additionally, the doctor may check for reduced blood flow, abnormal sensation, or tenderness in the surrounding tissue, which can reveal how widespread the damage might be.
Imaging Tests
Imaging is crucial for detecting necrosis that affects deeper tissues or internal organs:
- X-rays: Can reveal gas formation in tissues, especially in gangrenous necrosis, or involvement of bones in severe cases.
- CT Scans: Provide detailed cross-sectional images to evaluate the depth and spread of necrotic tissue, detect fluid collections, and guide surgical planning if needed.
- MRI: Offers high-resolution imaging of soft tissues, making it particularly useful for detecting early necrosis in muscles, the brain, or organs like the liver and kidneys.
- Ultrasound: Helps identify fluid accumulation, abscesses, or changes in soft tissues without exposing patients to radiation.
Laboratory Tests
Laboratory investigations provide additional information about tissue death and its underlying cause:
- Blood Tests: Elevated white blood cell count or markers like C-reactive protein (CRP) can indicate inflammation or infection. Organ-specific enzymes, such as liver or heart enzymes, may point to necrosis in those organs.
- Tissue Biopsy: A small sample of affected tissue can be examined under a microscope to confirm cell death, distinguish necrosis from other conditions, and sometimes identify the type of necrosis.
- Culture Tests: If an infection is suspected, samples of tissue or fluid can be cultured to identify bacteria, fungi, or other pathogens responsible for the tissue damage.
Specialised Diagnostic Approaches
For certain organs or complex cases, additional diagnostic tools may be required:
- Angiography: A test that visualises blood vessels to detect blockages that may have caused ischemic necrosis.
- Nuclear Scans: Highlight areas of reduced blood flow or tissue activity, helping identify affected organs or regions early.
- Other Functional Tests: Depending on the organ involved, heart function tests, kidney function tests, or neurological assessments may be used to evaluate the broader impact of necrosis.
How is Necrosis Treated?
Treatment for necrosis depends on the type, severity, and location of tissue death. The primary goals are to remove dead tissue, prevent infection, and restore blood flow.
Surgical Removal of Dead Tissue
One of the most common treatments is debridement, which involves surgically removing dead or damaged tissue. This prevents the spread of infection and promotes healing in the surrounding healthy tissue. In severe cases, such as gangrene affecting limbs, amputation may be necessary to protect the rest of the body.
Antibiotic or Antifungal Therapy
If necrosis is caused or complicated by an infection, targeted antibiotics or antifungal medications are prescribed. These help control bacterial or fungal growth, reduce inflammation, and prevent the infection from spreading to other parts of the body. Early use of medication is often critical to preventing life-threatening complications like sepsis.
Procedures for Restoring Blood Flow
In cases where necrosis is due to poor circulation or blocked blood vessels, doctors focus on restoring blood flow. This may involve procedures such as angioplasty, bypass surgery, or medications to improve circulation. Improving blood supply helps prevent further tissue death and supports healing in partially affected areas.
Hyperbaric Oxygen Therapy
Hyperbaric oxygen therapy involves breathing pure oxygen in a pressurised chamber, which increases oxygen delivery to damaged tissues. This method can be particularly helpful for certain types of necrosis, such as diabetic foot ulcers or gas gangrene, by promoting tissue repair and slowing the spread of infection.
Supportive Care
Supportive care is essential in managing symptoms and supporting the body’s recovery. This may include pain management, wound care, fluid replacement, and monitoring for complications such as organ dysfunction or systemic infection. Nutritional support and physical therapy may also aid in healing and recovery.
When Should You Seek Medical Help?
If you experience any of the following symptoms, it's important to seek medical attention promptly:
- Visible Changes in Skin or Tissue: Seek help if you notice sudden discolouration, blackening, unusual firmness or softness, blisters, open wounds, or foul-smelling discharge. These are often early signs of necrosis.
- Persistent Pain or Numbness: Continuous pain, tenderness, tingling, or loss of sensation in any area may indicate underlying tissue death or nerve involvement and should be evaluated promptly.
- Signs of Infection: Redness, swelling, warmth, pus, or foul odour around a wound, accompanied by fever or chills, requires urgent medical assessment to prevent sepsis.
- Organ-Specific Symptoms: Difficulty breathing, chest discomfort, confusion, weakness, or other sudden changes in organ function may indicate necrosis in vital organs like the heart, brain, or kidneys. Immediate medical care is crucial.
- Slow-Healing Wounds: Wounds that do not heal or keep worsening over time, especially in individuals with diabetes or poor circulation, should be checked for possible necrosis.
- High-Risk Conditions: People with diabetes, vascular diseases, severe infections, or compromised immunity should be especially vigilant and seek medical advice at the first sign of abnormal tissue changes.
Consult Today
If anything we've talked about today sounds familiar, whether it's a wound that's not healing right, or some unusual skin discoloration, don't brush it off or wait to see if it gets better on its own. At Max Hospital, our general surgeons and wound care specialists are experienced in assessing tissue health, managing necrosis, and will guide you through the right treatment options.
Frequently Asked Questions
Can necrosis be reversed or healed naturally?
Once tissue becomes necrotic, it cannot be reversed because the cells are already dead. However, early detection can prevent the spread of necrosis, and medical treatments like debridement, infection control, and improved circulation can help the surrounding healthy tissue recover.
Are certain people more at risk of developing necrosis?
People with conditions like diabetes, vascular diseases, immune system disorders, severe infections, or those who experience prolonged pressure on tissues (e.g., bedridden patients) are at higher risk of developing necrosis.
How quickly can necrosis progress?
The speed of necrosis varies depending on the cause. Infections and severe ischemia can lead to rapid tissue death within hours to days, whereas pressure-induced necrosis or minor circulation issues may develop over weeks. Early recognition is key to slowing progression.
Can necrosis affect internal organs without visible signs?
Yes, necrosis in internal organs like the heart, liver, or brain may not show visible external symptoms. Organ-specific signs, such as chest pain, shortness of breath, neurological deficits, or changes in liver or kidney function, may be the only indicators.
Is necrosis contagious?
Necrosis itself is not contagious. However, if it is caused by an infection, the underlying bacteria or fungus may be contagious under certain conditions, making proper medical care and hygiene important.
What lifestyle changes can help prevent necrosis?
Maintaining good circulation, managing chronic conditions like diabetes, practising proper wound care, avoiding prolonged pressure on tissues, and seeking early treatment for infections can reduce the risk of necrosis.
How long does recovery take after treatment for necrosis?
Recovery time depends on the severity, location, and treatment type. Minor necrosis with prompt treatment may heal in a few weeks, while severe cases involving surgery or organ damage may take months and require ongoing care.
Can necrosis recur after treatment?
Recurrence is possible, especially if underlying risk factors like poor circulation, diabetes, or repeated injuries are not managed. Regular check-ups and preventive measures are important to minimise the risk.
Written and Verified by:

Related Blogs

Dr. Vandana Boobna In Internal Medicine
Nov 08 , 2020 | 2 min read
Blogs by Doctor

What is Anaemia: Symptoms, Causes & Prevention Strategies
Dr. Namrita Singh In Internal Medicine
Jul 29 , 2024 | 3 min read

Typhoid Fever Symptoms, Diagnosis, and Debunking Common Myths
Dr. Namrita Singh In Internal Medicine
Jul 31 , 2024 | 2 min read
Most read Blogs
Get a Call Back
Related Blogs

Dr. Vandana Boobna In Internal Medicine
Nov 08 , 2020 | 2 min read
Blogs by Doctor

What is Anaemia: Symptoms, Causes & Prevention Strategies
Dr. Namrita Singh In Internal Medicine
Jul 29 , 2024 | 3 min read

Typhoid Fever Symptoms, Diagnosis, and Debunking Common Myths
Dr. Namrita Singh In Internal Medicine
Jul 31 , 2024 | 2 min read
Most read Blogs
Specialist in Location
- Best Internal Medicine Doctors in India
- Best Internal Medicine Doctors in Ghaziabad
- Best Internal Medicine Doctors in Shalimar Bagh
- Best Internal Medicine Doctors in Mohali
- Best Internal Medicine Doctors in Patparganj
- Best Internal Medicine Doctors in Saket
- Best Internal Medicine Doctors in Bathinda
- Best Internal Medicine Doctors in Panchsheel Park
- Best Internal Medicine Doctors in Dehradun
- Best Internal Medicine Doctors in Noida
- Best Internal Medicine Doctors in Lajpat Nagar
- Best Internal Medicine Doctors in Gurgaon
- Best Internal Medicine Doctors in Delhi
- Best Internal Medicine Doctors in Nagpur
- Best Internal Medicine Doctors in Lucknow
- Best Internal Medicine Doctors in Dwarka
- Best Internal Medicine Doctor in Pusa Road
- Best Internal Medicine Doctor in Vile Parle
- Best Internal Medicine Doctors in Sector 128 Noida
- Best Internal Medicine Doctors in Sector 19 Noida
- CAR T-Cell Therapy
- Chemotherapy
- LVAD
- Robotic Heart Surgery
- Kidney Transplant
- The Da Vinci Xi Robotic System
- Lung Transplant
- Bone Marrow Transplant (BMT)
- HIPEC
- Valvular Heart Surgery
- Coronary Artery Bypass Grafting (CABG)
- Knee Replacement Surgery
- ECMO
- Bariatric Surgery
- Biopsies / FNAC And Catheter Drainages
- Cochlear Implant
- More...




